- All You Need to Know
- Home
- SLIPPED DISC
- Slipped Disc Rules
- Lower back surgery
Lower back surgery
Lower back surgery asks what is the chiropractic take on the subject?
When to consult a surgeon?
Lower back surgery should only be considered when all else fails and you simply have nowhere else to turn. And the pain or disability is so bad that you just can't live with it any longer.
And then only if the surgeon is absolutely sure he knows where the pain is coming from. You see, Medicine's own term is FBS; Failed Back Surgery. Their own research indicates that less than 50 percent of fusions for example can be considered successful.
A group of the world's leading orthopaedic and neurosurgeons, with all the best tools and scanners available, concurred that they were less than half of the time absolutely sure what was causing the pain.

- Chiropractic Conditions is a central page at our site. It provides you simply and easily with the sorts of diagnoses that the average DC would be treating.
- Healthy Living Tips is another vital page at Chiropractic Help. Sparkling wellbeing is not just about having your subluxations adjusted. This link gives you some insights into different foods you could and perhaps should be eating.
Lower back surgery
Lower back surgery admits that when all else fails sometimes you may have no other option. Failed back surgery is a reality.
Distressing...
Over the years it has been a sobering fact that I've treated some patients with lower back and leg pain, not succeeded and eventually referred them to a medical specialist. The report comes back: The MRI confirms that the problem was at a different level from the one I was treating. Had I had access to that information in the beginning, I'm convinced at least half the time I could have saved the patient from lower back surgery, and his insurance a vast sum of money. One, a dear friend, is a constant reminder of how I screwed up. I was adjusting the wrong level. And now, after multiple surgeries, her life is miserable...
It's stretching the point but say for example you came to me with a Carpal Tunnel Syndrome in your right arm, and I treated your left arm. Would the right arm get better? Of course not. Likewise, if your chiropractor, or the surgeon, is treating say the L4-L5 facet on the right when the problem is was actually at the L2-L3 facet, would the patient get better? Certainly not.
Thorough examination
For both the chiropractor and the surgeon there is simply no substitute for a careful, conscientious and painstakingly-thorough examination. If you think your practitioner, chiropractic or medical, is doing anything less, GO ELSEWHERE! Knowing "what and where" is absolutely crucial.
TREATMENT BASED ON A WRONG DIAGNOSIS IS DOOMED TO FAIL, be it LOWER BACK SURGERY or CHIROPRACTIC ADJUSTMENTS.
ON WHAT BASIS WILL YOUR CHIROPRACTOR MAKE HIS/HER DIAGNOSIS?
The Physical Examination: before LOWER BACK SURGERY
Carefully and thoroughly, your doctor should:
- RANGE OF MOTION: Take you through the ROMs of your lumbar spine. Simply discovering that it is right lateral flexion that cause the pain to shoot down the back of your right leg gives a huge amount of information.
- ORTHOPAEDIC TESTS: There are many specific tests that have been developed over the years to distinguish between a facet syndrome, a disc syndrome, a sacroiliac syndrome ... and the treatment for the three is quite different.
- NEUROLOGICAL TESTS : Discovering that the numbness in the leg is in the groin and upper thigh, and not the side or back of the leg also gives us more vital information about the level of the lesion.
WRONG DIAGNOSIS = INAPPROPRIATE TREATMENT = FAILED BACK SURGERY/ FAILED BACK CHIROPRACTIC.
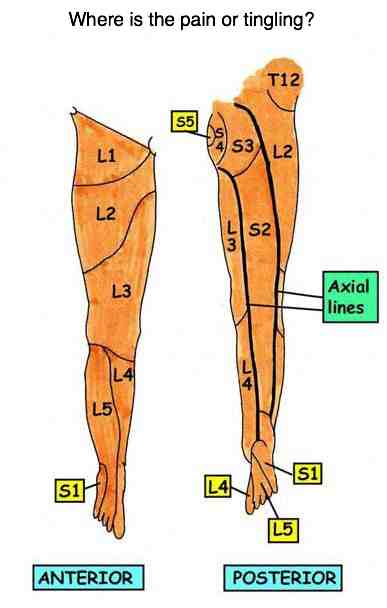
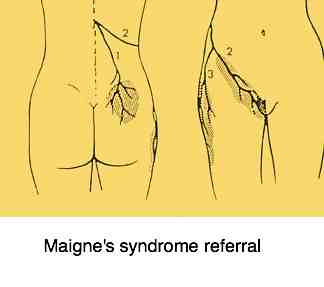
See how the ubiquitious Maignes syndrome can produce pain in the buttock, the side of the leg and the groin? Knowing exactly where the numbness is can make all the difference in arriving at an exact correct diagnosis: A facet syndrome on the right at L1-L2, or is it at L2-L3. Adjusting, or surgically treating the wrong level is doomed to failure.
REFLEXES and specific MUSCLE WEAKNESS
Likewise the reflexes and paresis of a particular muscle group give the clinician great insight into the level of the lesion. You can test yourself for muscle weakness...
4. Pain : Palpation of the segment can be very misleading, but it is one more tool that we use. If after all examinations there is still doubt whether the lesion is at L4-L5 or L5-S1, and L5 is very painful on palpation, then one might decide to go for the lower level.
5. Motion Palpation :
This is where your chiropractor will excel since s/he examines every
patient, looking for spinal fixations. Diligent motion palpation is a
powerful tool, but it too is not always conclusive. In a severe disc
lesion one may find no fixation at all, because the nucleus pulposis has
escaped the confining ring-shaped 'annular' disc fibres. And sometimes
an old injury resulting in a chronic fixation may give misleading
information about the current problem.
Radiological examination:
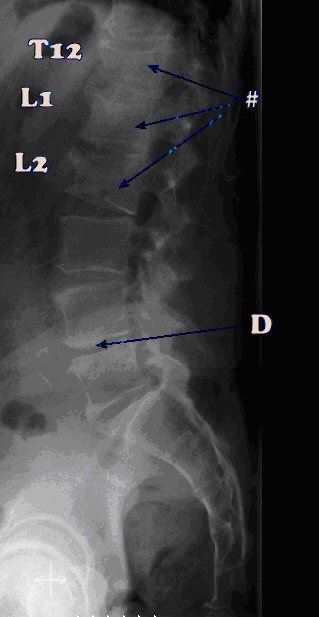
X-rays are both very useful, and can be very misleading. This particular patient has three compression fractures at T12, L1 and L2, (assumed medically to be the source of his pain), and loss of the L4-L5 disc space (marked D), yet Motion Palpation, Kemp's Test and deep tenderness indicated that his agony was coming from the facet joints at L5-L1.
A lumbar facet syndrome.
The proof of the pudding is always in the eating. Indeed adjusting L5 has decreased his pain and increased his mobility by 90%. This 64-year old man does his exercises faithfully, knows that he can't go on long dawdles with his wife when shopping, as he will the one to drop though a good 'wandel' is fine.
He comes in every six weeks for his maintenance treatment. This man was under threat of lower back surgery, and is more than happy with Chiropractic.
I wonder on which part of his spine they were planning the surgery? Where the fractures are? At L4-L5 where the disc space is reduced? Or at the actual level of his problem: L5-S1?
MRI SCAN
LOWER BACK SURGERY
It's widely acknowledged by radiological researchers that a significant (up to a third) of normal people with absolutely no back pain have bulging discs and abnormalities on MRI. Having said that, the MRI is a wondrous tool, fiendishly difficult to read properly, but it can make all the difference in coming to a sound diagnosis.
Unfortunately, an
unethical surgeon, or chiropractor for that matter, looking for a fast
buck can usually find something on MRI or X-ray that can be used to
convince you that his/ her procedure will help you.
"It's critical to have a thorough workup — to get a sense of the root cause of your pain."
Arnold J. Weil, M.D.
Chiropractic help
Research shows that if you first consider chiropractic help then you are much less likely to go for lower back surgery.
Yesterday I was consulted by a young man with severe pain in the back of his right thigh and calf. The pain started three months previously in his back for no obvious reason. As the pain in his leg increased, so lower back pain receded:
20% LBP / 80% leg pain, an ominous sign.
Worse,
the "crossed" Slump test was strongly positive. Raising his LEFT leg
produced severe pain in the back of his RIGHT thigh.
Aside: If the crossed sign is strongly positive, traction will always aggravate the condition.
He stood in an antalgic posture, stuck forwards and leaning towards the side of pain. The so called Dejeurine triad was positive: coughing, sneezing and bearing down on the WC were painful.
Surprisingly there were no hard neurological signs; no numbness, normal reflexes and no muscle weakness.
The lowest segment in his back, normally L5, was exquisitely painful on palpation, and fixated on motion palpation.
Is this a simple straight forward diagnosis? Postero Medial L5 S1, Grade II lumbar disc protrusion.
Not so. One look at his X-rays show an extra lumbar vertebra (a so-called "lumbarisation" of part of his sacrum S1, with loss of L4-L5 disc space. So, is the problem at L4-L5 or L5-L6 or L6-S1?
X-rays point to the higher level, examination to the lowest. The presence of the anomaly makes the pain pattern to the back of the thigh less certain. Today he has a MRI scan, out of his own pocket because his doctor has refused to order a scan.
Knowing the level of the lesion, with a high degree of certainty is critical to a successful outcome. Three months of medical management (neglect frankly, in my opinion) has seen him get steadily worse. Can Chiropractic still mean something for him at this late stage? Or is it lower back surgery?

What's on his side is that the Postero Medial disk herniation usually
responds better and quicker than it's more common first cousin, the
Postero Lateral Disk herniation.
POSTERO MEDIAL DISK HERNIATION ...
4 days later we have the MRI
It came as no surprise. A large lumbar disc protrusion at L5-S1, the lumbarisation, the list to starboard, and the pinched nerve in the foramen. Exactly what the physical exam predicted.
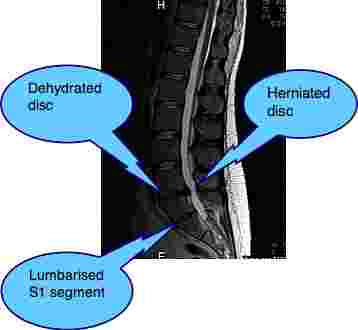
See how the young man has an antalgic list TOWARDS the painful side. What I call the Pisa sign. This is typical of the postero-medial disc herniation. Exactly what I expected.
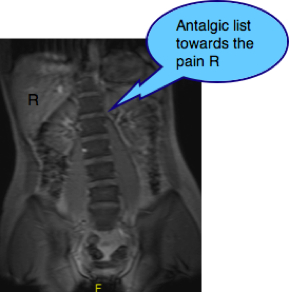
Here you can see the large bulge into the foramen trapping the nerve to the back of his right leg. No wonder he has so much pain in his thigh. This is sore. Ouch!

This is a serious case. Medicine says we have no business dealing with a case like this. He should go straight under the knife.
I give him a 50/50 chance of escaping surgery. Everything is dependent on "does he trust me". Will he go the distance, or will family and friends, his doctor, pressure him? One sneeze, one silly movement can change everything.
Minus: He had a lot of pain after the first treatment, and had to call his doctor in for a shot.
Plus: Today, lifting his left leg produced no pain in his right leg. He too noticed it straight away. But, he's on heavy medication.
My take? He's definitely a bit better, but it's a knife edge. This is what makes Chiropractic so exciting. The challenge, the human drama. Never bored, I'm exhausted 's avonds. I'm a Dutchman. In the evening.
When he's at home, he SHALL follow these rules to the T. No set backs is the rule:
SLIPPED DISC RULES ...
LOWER BACK SURGERY COSTS
Americans spend $86 billion on back treatment every year, roughly the same as for cancer, a very large slice of which goes towards the back surgery costs. However research confirms that the problem is getting worse not better despite all the moola spent. Discectomies and fusions are soaring, over one million per year in the USA, yet more and more people are disabled and miserable.
8% of patients have a second surgery within two years; and 20% within ten years. Less than half of fusions are appropriate and successful. At a cost of $75,000 each...
Chiropractic costs
I give the young man in the case above about a 80% chance of full recovery, if he sticks with the program. He has a surgical consult in a month, and I have to do a miracle before that. 80% is admittedly a thumb suck, but based on thirty years experience. The direct cost?
Acute phase: 2/w for 4 weeks = 8 treatments.
Rehab phase: 1/w for 3 weeks = 3
Tailoring off 1/w 2 weeks = 2
Maintenance: 1/6w for 40 wks = 7
20 treatments in one year @ €43 = €700 - €1000
The "intangible costs" are more difficult to measure. He has his own computer business and will be completely out of action for at least a week, as he may not sit, not at all. Thereafter he will most likely be able to perch and do some time on his computer. In total he is probably going to be disabled and unproductive for 2-3 weeks. One sneeze can change everything...
Prestigous medical journal "Spine"... LOWER BACK SURGERY

‘Spine’ is probably one of the most esteemed medical journals in the world. Spine has reported that, in a randomized controlled trial or RCT (one of the benchmark Chiropractic research trials) of patients with chronic back and neck pain, after 9 weeks of Chiropractic treatment 27% were completely without pain. In comparison only 9% of patients who received acupuncture and a miserly 5% of patients who took prescribed medication were pain free.
In another Spine research article Aure et al showed that in a group of 49 patients with chronic low back pain, preventing them from working, that 67% of those receiving manipulation were back at work after two months in comparison with 27% who received exercise only.
CHIROPRACTIC RESEARCH @ Bernard Preston.com ..
CHIROPRACTIC RESEARCH @ Chiropractic-Books.com
Use the site search function on your left to find these links.
Lower back surgery risk factors
- SMOKING: As in all surgery, smokers are at higher risk of Failed Back Surgery syndrome. There just isn't enough oxygen for the tissues to heal properly. Add to that the atherosclerosis narrowing the blood vessels. Add to that the coughing... And then of course you're at much higher risk from the General Anaesthetic if you are a smoker.
- OBESITY. Presenting his research done at Jefferson University hospital, neurosurgeon Dr John Ratliff found a much higher incidence of complications in extremely overweight and obese patients, including blood clots, wound infections, heart problems, and deep vein thrombosis. “We found that the incidence of complications related directly to the degree of obesity,” he says...
- DIABETES. It's well known that diabetics, particularly poorly controlled diabetics, have a higher risk of wound infection and complication in all forms of surgery. Consider walking benefits both to prevent lower back surgery and maintain better blood sugar levels. A leg length inequality should be considered if standing and walking increase the pain... WALKING BENEFITS ...
Every Chiropractor will tell you how s/he dreads the acute low back and leg pain patient who is also a smoker. The chances of chiropractic helping, are also reduced...
ATHEROSCLEROSIS SYMPTOMS Low Back Pain ..
LEG LENGTH INEQUALITY ... a short leg?
To find links to the topics in bold copy and paste them into the site search function in the navigation bar on your left.
BACK SURGERY COSTS
When considering lower back surgery costs, one must also count in the hidden costs: the months of sick leave and loss of productivity, the decreased enjoyment of life for the patient with lower back pain, the rehabilitation, and the burden borne by the whole family, when one member goes 'man down' for a few months. Read more in this report: LOWER BACK PAIN ..
LEG PAIN AFTER BACK SURGERY
If at all possible avoid LOWER BACK SURGERY
I don't pretend to have the statistics as to just how often leg pain develops AFTER surgery (I'm on the hunt for them and will update this page accordingly) but in practice one is fairly regularly faced with patients who either got little relief of leg pain, or temporary relief, or leg pain started after surgery.
Can that happen with
Chiropractic too? Yes, it can, though the incidence in my own practice
is low, and almost always of a temporary nature. Chiropractic
researchers are now busy gathering statistics of this nature so that we
have a much clearer science-based answer, rather than a general thumb
suck.
LEG PAIN after BACK SURGERY ...
TO SUM UP... LOWER BACK SURGERY.
I'm personally in principle not against good lower back surgery based on a sound diagnosis, after all else has been explored, and in the hands of a careful and experienced surgeon. I refer patients myself for surgery occasionally when it's clear that Chiropractic is not going to help.
A surgeon would probably say: ... I not against Chiropractic care ... in the hands of a careful and experienced chiropractor...
How do Chiropractors and Surgeons become competent and experienced. The hard way, I'm afraid. We don't call it 'a practice' for nothing. We practice on you!
Careful, thorough and conscientious are not necessarily qualities that one gains with experience. I personally think that all patients, no matter what condition they have, should be asking themselves the question: "Is this doctor, chiropractor, surgeon... being careful, thorough and conscientious?" If you're unsure, vote with your feet!
"A teacher is one who makes himself progressively unnecessary."
Thomas Carruthers
A good doctor too.
Complications of surgery
Before going for lumbar back surgery it's worth giving chiropractic
treatment a solid try. At least a month. Obviously there are
exceptions...
COMPLICATIONS OF SURGERY ...
LOWER LUMBAR BACK PAIN
Avoid LOWER BACK SURGERY
Successfully addressing chronic lower lumbar back pain in the chiropractic clinic usually means addressing numerous factors: a short leg, spinal and sacroiliac and hip fixations, poor muscle tone, obesity, smoking, posture and work situations... all contribute to back pain. LOWER LUMBAR BACK PAIN ..
The above case...
Fortunately there were two people very determined that he wouldn't have lower back surgery. He and I. Despite the pain he needed no encouragement to go the distance.
Unlike medicine in chiropractic the patient is very involved in the healing process. It's not just a case of take a pill, and go on with your life... it's vital that you follow instructions to the letter, use your common sense. In a sense it's your own body that is the healer, all we are doing is aiding and abetting that process. Refusing to do the exercises faithfully, to stop sitting, even one good sneeze can ruin everything.
Prevention is the key...
Lower back and leg pain
Lower back and leg pain is the most common complaint at chiropractic clinics; it doesn't mean you are entirely excluded from lower back surgery, but the chances are significantly lower.
A cure?
There's a perception in the minds of some that after lower back surgery one will finally have a cure for all that pain. Sadly that's not true, not after you've been to the surgeon, nor after the chiropractor.
A cure simply doesn't exist with most medical conditions, and that includes lower back and leg pain. Continued treatment and management of one sort or another remains imperative, and a disciplined set of exercises; otherwise it's only a matter of time before the second and perhaps more lower back surgery.
Whilst not wanting to be neurotic, due care remains important. Falls happen, but playing silly buggers is just plain stupid. Read more for example about this case of severe groin pain, numbness and tingling from the knees up to my buttocks after an unscheduled fall.
USEFUL LINKS @ LOWER BACK SURGERY
- Home
- SLIPPED DISC
- Slipped Disc Rules
- Lower back surgery
Did you find this page useful? Then perhaps forward it to a suffering friend. Better still, Tweet or Face Book it.
