- All You Need to Know
First rib syndrome

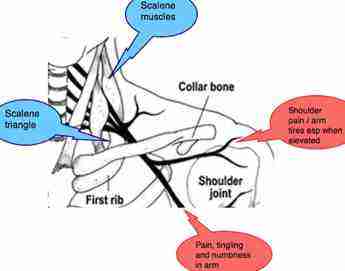
First rib syndrome causes pain and tingling in the arm.
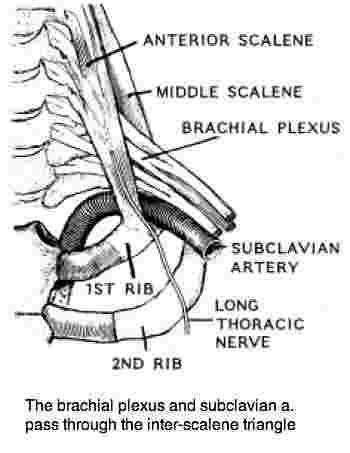
Inter-scalene triangle
The inter-scalene triangle is an easy to visualise two dimensional structure bounded by the anterior and medial muscles and the first rib below. Through this narrow passage both the brachial plexus and subclavian artery pass on their way from the chest to the arm.
Thus compromise of this space can cause both neurological and or vascular signs and symptoms giving a complex and often confusing pattern of shoulder and arm pain, paresthesias in any part of the arm and radiating potentially in a non dermatomal pattern to all fingers.
The arm tires easily, especially with overhead use, and may feel cold and become pale. Many of the shoulder and arm conditions treated in chiropractic clinics have a chronic thoracic outlet syndromes as their underlying cause. For example, frozen shoulders, tennis elbow ...
- frozen shoulder; a debilitating and very painful condition
- tennis elbow; it can last for years if the underlying cause is a low grade Thoracic Outlet Syndrome
- carpal tunnel casefile, an underlying first rib fixation.
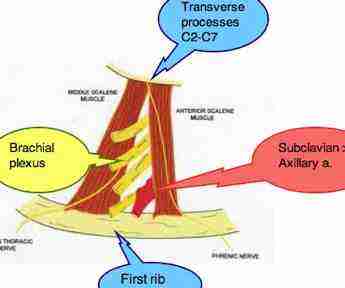
The scalene muscles
The anterior and medial scalene muscles that bound the inter scalene triangle, we will ignore the posterior scalene, have the transverse proceses of the c2-c7 as their origin, and insert onto the first rib.
They are an accessory to breathing, raising the first rib, and also laterally flex the neck to the same side.
They are innervated by c3-c6.
The triangle may be palpated by rotating and laterally flexing the head and neck to the opposite side, and gently running the fingers posterior to the sterno cleido mastoid muscle, following the scalenes caudally as they descend deep behind the clavicle to their insertion on the first rib.
The thoracic outlet is far more difficult to visualise, being a three-dimensional structure. As the subclavian artery, becoming the axillary artery, and the brachial plexus emerge from the inter scalene triangle, they pass between the first rib and the clavicle on their way to the shoulder and thence to the whole arm and hand.
On the way, they pass under the tendon of the pectoralis muscle, which we will see can have significance.
Cervical rib
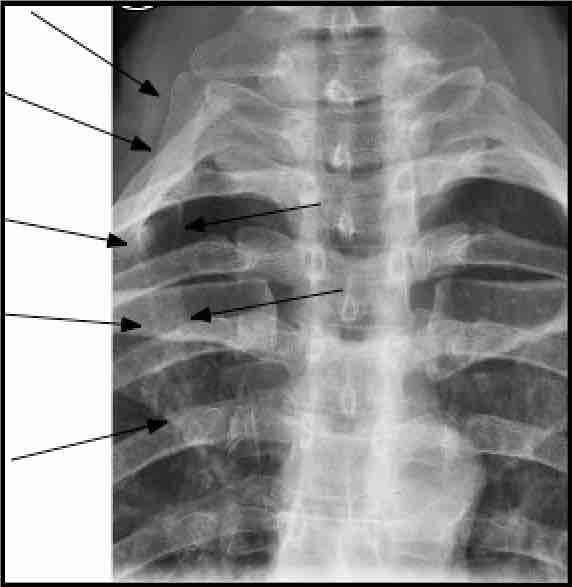
The brachial plexus (C5-T1) may be irritated and occasionally physically compromised as it emerges from the Scalene Triangle, either by the first rib, or hypertrophy or spasm of the scalene muscles, or the clavicle, or by any structure that invades this space.
A cervical rib, very occasionally an apical lung tumour (Pancoast, for example), or scar tissue from old injuries may invade the interscalene space. Old fractures of the first rib, or the clavicle may set up compression of the artery or nerves as scar tissue grows around the fractured bone.
First rib fixation
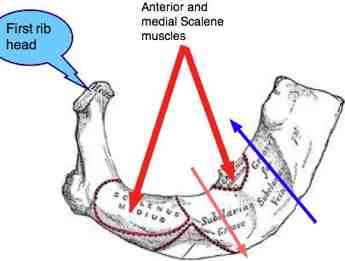
Note that the subclavian artery passes through the interscalene triangle, but the vein, in blue, doesn't. There are grooves in the first rib to accomodate the artery and vein.
Normally, the first rib should descend on exhalation as the scalenes relax. However, either a first rib fixation, or scalene spasm may prevent the rib descending.
The first rib articulates posteriorally with a single facet with the body of T1 and anteriorally with the sternum via a costal cartilage allowing for limited movement of the rib in inspiration and expiration.
A (left, say) first rib fixation may be detected by rotating the head to the SAME side with the right hand, palpating the body of the left first rib (in its central part) and then gently depressing the rib with the left fingers whilst simultaneously laterally flexing the neck to the SAME side (to reduce upward scalene traction on the rib).
Normally, you can feel the rib depressing under the pressure of the fingers. When fixated it has a hard rigid feeling. The examiner shoulder then palpate along the length of the first rib to determine if the fixation is more at the costo-sternal, or costo-thoracic joints.
VASCULAR symptoms
Occupations that involve lifting the arms for long periods, such electricians, hairdressing, playing a musical instrument such as the violin or clarinet, and carrying a backpack... close down the space between the clavicle and the first rib, and may compromise the thoracic outlet.
Typical vascular symptoms would include fatigue when using the arm. In effect an intermittent claudication. At rest there are minimal vascular symptoms, but on use of the arm, especially with the arms raised when the arterial system is even further compromised in the Thoracic Outlet, and ischemia soon occurs.
First rib syndrome
First rib syndrome also causes the arm to tire quickly especially above the head as in hanging washing.
Pectoralis minor muscle
Further laterally, the neurovascular bundle passes between the Pec Minor tendon and the chest wall. In cases of hypertrophy and chronic tendonitis they may be compromised, again especially when the arm is elevated.
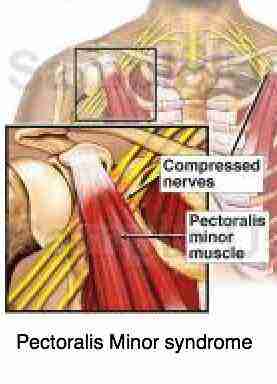
The axillary artery also passes beneath the Pec Minor tendon.
Cervical ribs
About 2 people per thousand have an extra cervical rib, located above the normal first thoracic rib. This cervical rib penetrates through the inter scalene triangle, taking up space and when large can produce severe signs and symptoms in the arm.
Symptoms of first rib syndrome
When the subclavian / axillary artery is affected primarily, the arm quickly tires, especially as stated previously with the arm elevated, and the head extended and laterally flexed to the opposite side (watching where the worker is drilling/ working). The arm may feel cold and may have pins and needles. The differential should include Carpal Tunnel Syndrome, but the paresthesias then are only in the Median nn. distribution.
The subclavian vein is rarely affected as it normally passes anterior to the Scalene Triangle. However, a normal variant can occur with the vein exiting the Thoracic cage via the Scalene Triangle, in which case the arm may swell. Thrombus formation must be ruled out. I've have personally only seen one case in thirty years.
When the brachial plexus is affected primarily, there is often a vague dull, diffuse ache in the shoulder, arm and hand. Symptoms are of an intermittent nature. A key indicator is involvement of all fingers, though the lowest nerve trunks, which pass directly over the first rib, are most often affected, or worst affected, so the C8-T1 dermatomes are affected predominantly. Paresthesias and numbness may occur with pain radiating down into fingers. Carrying heavy objects in the arm, such as a shopping basket and sleeping with the arm elevated above the head will aggravate the condition.
Conversely, a true brachial neuralgia with nerve root irritation or compromise is usually relieved by elevation of the arm. Shoulder Abduction Relief sign...
Diagnosis of first rib syndrome
Watson, et al (Manual Therapy 2009; 14: 586-595) point that the diagnosis is often one of exclusion, with Thoracic Outlet Syndrome being used as a "fallback diagnosis". In their opinion 98% of TOS cases are of the neurogenic type. Differentials should include:
- Carpal tunnel syndrome
- DeQuervain's tenosynovitis
- Lateral epicondylosis
- Complex regional pain syndrome (whatever that is!)
- Horner's syndrome,
- Raynaud's disease
- Cervical Radiculopathy
- Brachial plexus trauma (a stinger)
- Deep vein thrombosis
- Rotator cuff and glenohumeral pathology.
Arm Pain Quick DASH questionaire
DASH: Disability - Arm - Shoulder - Hand
This questionaire quickly gives the clinician an inkling of how severe the patient's compaint is, and which activities are likely to increase the symptoms. It's useful for the patient to download the questionaire, and fill it in before the first consultation. Arm pain Quick DASH questionaire.
Clearly examination should be comprehensive and include the cervical spine, shoulder, elbow, wrist and hand.
Adson's test
For me the diagnosis of First rib syndrome is confirmed by a positive Adson's Test, but it remains a subjective, and difficult to perform manoeuvre.
I personally find that in a frank case of Thoracic Outlet Syndrome it is not necessary to extend the arm (that is controversial and not standard practice!), (since the pulse is often obliterated in healthy subjects when extending the arm, giving many false positives.)
And I add an extra proviso...
If the pulse is obliterated by rotation of the head and neck to the same side, extension of the head and neck, and deep inhalation, AND THE PULSE RETURNS UPON RETURNING THE HEAD TO THE NEUTRAL POSITION AND EXHALING, then I am reasonably sure of the diagnosis of TOS.
To summarise: I make a diagnosis of Thoracic Outlet Syndrome if at least three of the following are positive:
- A case history that is consistent with the TOS pattern of symptoms described above.
- Tenderness in the supraclavicular space and/ or a fixation of the first rib.
- Active trigger points in the anterior and/or medial Scalene muscles.
- A positive Adsons test.
The Hands-Up test

This rather brutal test comes in two forms:
- Position I: Raise the arms in the "hands up" 90/90 position, palms forwards, in the coronal plane. The patient is then asked to clench and unclench their fists for three minutes.
- Position II: Exactly the same but with the shoulders extended (as in carrying a backpack), closing down the costo-clavicular space.
A positive test: a deep numb ache in the arms (that I have myself after three minutes, in the extended position, and I definitely don't suffer from THORACIC OUTLET SYNDROME!), pain or tingling in the fingers and arms, or an excessively tired arm.
My own opinion is that if the diagnosis is based on Hands-up test, particularly with the shoulders extended, then half the world will be found to be suffering from Thoracic Outlet Syndrome!

Costo-Clavicular manoeuvre for first rib syndrome
Placing one's fingers in the supraclavicular space it is easy to palpate the first rib approximating the clavicle as the abducted arm is flexed and extended.
In the CostoClavicular manoeuve, the doctor seeks a strong radial pulse, extends the arm and depresses the shoulder, waiting for a cessation of the pulse.
In a true positive, for my money, the radial pulse should return when the arm is returned to neutral.
Upper limb tension test
The ULTT is normally used as a test for a nerve root impingement. However it is equally useful in first rib syndrome though less profoundly positive, giving a tight feeling or ache in the forearm.
My own opinion
When examining the patient with a stubborn tennis elbow, frozen shoulder or Carpal Tunnel Syndrome, I frequently find both a first rib fixation and a positive Adson's test. I believe it to be the adjustment of the first rib fixation that gives Chiropractic the edge in the management of these arm and shoulder conditions. Though there is no research confirming that Chiropractic can help CTS, it's not often that I fail in the management of this sometimes stubborn and nasty condition. Oh for the time to test this with some solid blinded research.
An observation
Frequently it takes only one or two adjustments of the first rib to free the fixation. But... a mid-low cervical fixation is often then found. At first I doubted my palpation skills, but it occurs so frequently that I believe it be part of the syndrome.
My opinion? The cervical facet fixation sets up the Scalene spasm that leads to the typical Thoracic Outlet signs and symptoms. The the question arises: Is the fixated rib primary to the condition, the spasm in the scalenes causing the first rib fixation? Is it cause or effect?
An important question
Does the fixated first rib, and the development of THORACIC OUTLET SYNDROME set up the patient for a frozen shoulder for example.
Or is the frozen shoulder the cause of the fixated rib and scalene spasm?
Chiropractic management of these neck-shoulder-arm pain syndromes
The correct protocol is to fix what you find. If there's a fixated rib, then adjust it. If there's a capsulitis, or radial head fixation, or active trigger points in the Pronator teres... fix it by whatever tools one has.
Then, mostly, the patient gets better; alas, not always.
Did you find this page useful? Then perhaps forward it to a suffering friend. Better still, Tweet or Face Book it.
