- All You Need to Know
Wisdom teeth removal infection
Wisdom Teeth Removal Infection recommends you have them out in the chair; with no general anaesthetic.
This page was last updated by Dr Barrie Lewis on 20th January, 2019.
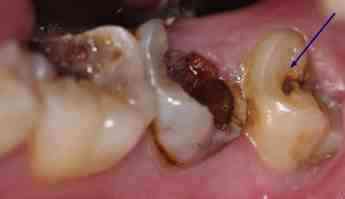
Infected and impacted wisdom, also known as third molar teeth cause difficulties with oral hygiene in the recesses of the mouth. Awkward to floss and brush, with food debris collecting between the tooth and the jawbone and gum, tooth decay is almost inevitable.
What to do with wisdom teeth remains controversial in the circles or oral surgeons. In some countries the practice of extracting them whether healthy, impacted, infected or not is prevalent. Other countries are less proactive waiting until they create a problem. Fiery debates continue. In the chair by your dentist? Under anaesthetic by an oral surgeon only? Money and defending of turf comes also into the equation.
The problem is that the lingual nerve, which supplies taste to the tongue. and the inferior alveolar nerve lie very close to the lower wisdom tooth. Research reveals that up to about 2 percent of surgical cases can produce serious injury to one or other of the nerves.
Part of the problem is that the position of the lingual nerve is quite variable, and, in 10 percent of cases is above the so called lingual plate creating difficulties for oral surgeons.
Another is that prolonged opening of the mouth can cause trismus or spasm of the muscles of chewing. Over opening of the TMJ can damage the meniscus within the jaw joint.
This month has seen three women in their thirties suffering from severe facial pain, TMJ dysfunction and painful migraine type headache after surgical procedures
in the mouth.
All three were treated under a general anaesthetic. Two developed the pain after wisdom tooth extractions, and one after a procedure for tonsils.
All
three had associated neck pain, and in one case the stiffness in the
neck raised suspicion of meningitis, resulting in a hospitilisation.
Eventually she was discharged after a negative lumbar puncture, but the
headaches and facial pain continued for some months. No one thought to examine the jaw joints, and the muscles associated with mastication.
Why do women appear to be more prone? This is purely anecdotal so I have no research to present about the sex distribution of facial pain after surgery in the mouth. But a woman has a smaller mouth, and can't open as wide, that's fact. And most dentists and oral surgeons are men, have large hands. Opening of the mouth
under anaesthetic, particularly for a prolonged period, when the patient is unable to protest, and you stand the possibility of facial pain syndrome which will mostly have associated headache and neck pain; the pain may be self limiting, and of a temporary nature, but sometimes in lasts for years.
If the wisdom teeth are not impacted then do your best to convince your dentist to pull your wisdom teeth in his office under local anaesthesia.
Wisdom teeth removal infection
Wisdom teeth removal infection under anaesthetic can cause severe life long TMJ dysfunction, facial pain and migraine.
With human jaw bones gradually becoming smaller, there is less space for the wisdoms, or third molars as dentists call them, and they have the propensity to crowd the adjacent molars causing them to malalign, both with neighbouring teeth and the molars from the opposing jaw. These crooked teeth are both visually not pleasing but more seriously it affects chewing and the harmony of the paired TMJs.
In addition,
they often impact or erupt only partially causing a host of
difficulties; more information on dentistry sites. In particular they
are often half covered by a flap of gum that makes wisdom teeth removal
infection almost inevitable. Food particles gets trapped under the flap
making it very difficult to clean the teeth properly.
Because
of their location remotely in nethermost nooks of the mouth, and the
fact that food particals tend to accumulate behind the wisdom tooth,
brushing and flossing is usually less effective. So, infection; pain,
redness, swelling affects the area locally, but the infection may also
spread into the bone and the jaw joint which lies very close by; the
pain and even spread to the cervical spine; the sensory nucleus of the
nerve that supplies the jaw is found in the neck, so you may feel mouth
related pain in the neck, strange as that may seem.
So, for dentists a frequent practice is wisdom tooth removal before infection. It's sensible, and I take no issue with the practice. Prevention is better than a cure in the mouth just as elsewhere in the body, especially as wisdoms often have smaller roots and can be easily extracted without the necessity of a general anaesthetic. In short, by your dentist in the chair in his or her clinic.
Controversy reigns about when is the optimum time. In some parts of the world wisdom tooth extraction is recommended as teenagers, even perfectly healthy wisdoms, before they inevitably cause infection; and before the jawbone becomes harder and thicker, making extraction more difficult and a greater likelihood of injuring the nerves and even the floor of the sinuses as the upper wisdom teeth come out.
In other words, before the infected wisdom, marked in the graphic above, begins to infect adjoining wisdoms as we may see happening.
The long and the short of it is that you are probably going to have all four wisdom teeth extracted, one way or another, sooner or later, if they haven't already been pulled.
Removal of wisdom teeth under a general anesthetic.
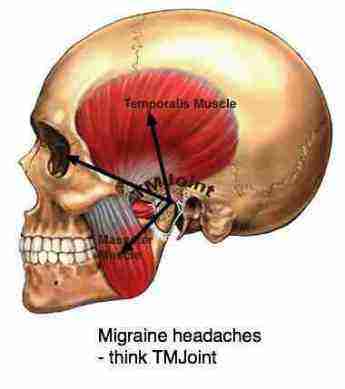
There certainly is a place for infected and impacted wisdom teeth removal under a GA, especially as the Lingual and Inferior alveolar nerves may be damaged during a difficult impaction.
This however needs to be the exception, not the rule; plead with your dentist to pull your infected wisdom teeth in the chair under a local anesthetic. Quite apart from the cost, which will be much higher under a general, but more important will less likelihood of injury to your TMJ.
Noscomial infection in hospital, dangers of a general... have your dentist pull them, unless he strongly recommends in your case you attend a surgeon. Which will happen occasionally.
In most instances it's routine to have a fully erupted wisdom pulled under a local in the chair. Squeal if s/he is over opening your mouth.
Here's an interesting Case history @ Wisdom tooth extraction and headache.
A 30 year old woman consulted me with right jaw joint pain, facial pain and severe headache, and upper cervical pain. Three months previously she had her wisdom teeth extracted under general anaesthetic.
On examination, there was extreme tenderness of the right TMJ with associated active trigger points in the right masseter, temporalis and external pterygoid muscles.
Fortunately there were no popping or clicking sounds from the TMJs, but there was delayed opening of the left TMJ.
Rotation of the neck, in both directions was painful, with a marked fixation of C2.
There were other details that I won't bore you with. It took six treatments of her upper cervical spine, jaw joint mobilisation and deep, painful soft tissue work of the muscles, to relieve her severe facial pain and headaches.
I'm hoping her condition will now stabilise; she's had to stop chewing gum. The next step is TMJ exercises. But there is no guarantee that this will not continue, and become chronic migraine and facial pain. If often does, but fortunately she didn't wait years before consulting me.
Popping and clicking jaw joints are not uncommon.
If the jaws are forced even wider, then the meniscus in the joint is injured, and the joint begins to develop a painful click, often associated with facial and jaw joint pain and headaches.
Prevention is the key. If at all possible, have them out in the chair.
TMJ dysfunction
Many folk are not aware that TMJ dysfunction can be at the root of their facial pain and migraine type headaches; or that it all began after wisdom teeth removal due to infection or impaction. Our jaws are getting smaller.
The popping, clicking and grinding sounds within the TMJ as we chew and speak is ignored; spouses often report hearing it whilst kissing too.
There are many causes by prime amongst them is over opening of the jaw under a general anaesthetic.
Migraine headache
Often it's assumed that migraine headache is caused by certain foods, weather changes, and exhaustion, for example. However, in the presence of definite TMJ dysfunction signs, a proper evaluation of the jaw joints is indicated. Not uncommon is that these popping sounds began after wisdom teeth removal infection.
Facial pain
Facial pain is a common sequela after wisdom teeth removal infection; in may be temporary, or become a life long problem.
Trigeminal neuralgia too needs to be considered.
Handy links
Did you find this page useful? Then perhaps forward it to a suffering friend. Better still, Tweet or Face Book it.
